Warning: This article discusses the issue of substance abuse and the resulting Tranq (Xylazine) sores. It may include graphic images of wounds that could be disturbing or triggering for some readers. Please proceed with caution.
Xylazine, commonly referred to as “Tranq”, originally debuted in veterinary medicine, serving as a dependable sedative for animals.
However, this seemingly innocuous substance has taken a dark turn.
The United States is now grappling with increasing concern over devastating wounds directly linked to Xylazine misuse.
The bridge from veterinary clinics to human trauma is a story that demands attention.
Background and Usage of Xylazine
“Tranq Dope,” commonly called “Tranq, ” is street slang for a drug combination containing the veterinary sedative Xylazine mixed with an opiate, usually Fentanyl.
While initially intended for sedating animals, the outcomes can be devastating when this concoction enters the human realm.
Tranq doesn’t just pose a threat of addiction or overdose; it also causes severe, ulcerative wounds that can lead to significant tissue damage.
These wounds aren’t your typical marks of drug misuse; they’re graphic, painful reminders of the drug’s potent and dangerous effects on the human body.1
It’s a stark testament to the hazards of veering from a substance’s intended use.
Understanding Tranq (Xylazine) Sores
Tranq sores are skin lesions associated with misusing Xylazine.
Xylazine is mixed with other substances, particularly Fentanyl, and injected; the combined effect can compromise blood flow to the area, exacerbating the skin’s reaction and leading to these sores.
These sores manifest as painful, open ulcers and can vary in size and severity.
Often surrounded by discolored or necrotic tissue, they present a stark visual representation of the drug’s harmful side effects on the human body.
When injected with Xylazine, a drug not intended for human consumption, it can lead to localized tissue death due to its acidic nature.
Beyond the physical damage, these lesions also have a heightened risk of secondary bacterial infections, leading to complications such as amputation if not treated promptly.2
The occurrence of Tranq sores is a poignant reminder of the dangers of Xylazine misuse and the broader issues related to adulterated street drugs.
Clinical Manifestations of Tranq Sores
When discussing the clinical manifestations of Tranq sores, it’s essential to understand their progression, appearance, and differentiation from other drug-induced complications.
Presentation
Appearance:
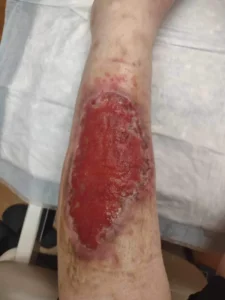
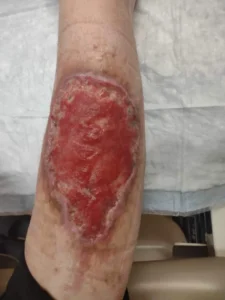
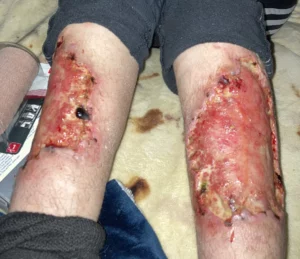
Tranq sores typically begin as redness or minor skin irritation, rapidly progressing to open ulcers with discolored or necrotic (dead) tissue.
These sores may have a weeping appearance, emitting fluid or pus, mainly if a secondary bacterial infection occurs.
Location:
The sores predominantly develop at the injection site.
In individuals who use Xylazine intravenously, common areas include the arms, legs, hands, or feet—wherever a vein is accessible for injection.
However, wounds have been documented in other places too, other than where injected.
Stages:
The progression often begins with skin irritation or a small bump.
If left untreated, or if the individual continues Xylazine misuse, the lesion can evolve into a full-blown ulcer with potential necrosis.
Deep tissue damage might be present in its most severe form, requiring extensive medical intervention.
| Characteristics | Description |
|---|---|
| Appearance | Tranq sores often manifest as linear or zigzag-shaped wounds on the skin. Their size and depth can fluctuate, going from shallow abrasions to profound ulcers. |
| Location | Tranq sores are usually found on parts of the body where injections are made, like the arms, legs, hands, or feet. |
| Pattern | The pattern of the sores may match the injection sites, suggesting repetitive use in the same spots. |
| Inflammation | Signs of inflammation such as redness, swelling, or tenderness might be seen around the Tranq sore. |
| Risk of infection | Because they are open wounds, Tranq sores heighten the risk of secondary infections, especially if one doesn’t maintain good hygiene and wound care. |
Differences from Other Drug-Induced Sores
Tranq sores, due to their association with Xylazine, tend to be more necrotic in appearance compared to other drug-induced lesions.
This means that the tissue decay is often more pronounced.
While many drug-induced sores, such as those from Methamphetamine use (“Meth Sores”), are often accompanied by compulsive skin-picking, Tranq sores usually arise more directly from the drug’s acidic properties and its impact on tissue blood flow.
The rapid progression from minor skin irritation to an ulcerative state is a distinguishing factor of Tranq sores.
Other drug-related sores may develop more gradually or due to a combination of factors like poor hygiene, malnutrition, or continued skin manipulation.
The location can also be a clue.
While many drug-induced sores can appear anywhere, Tranq sores predominantly manifest at injection sites.
Healthcare professionals must recognize these distinguishing factors in clinical settings to provide appropriate care and interventions for affected individuals.
Photos of Tranq Wounds (WARNING: GRAPHIC!)
The Dangers and Implications
The consequences of Tranq-induced sores are serious, affecting individuals both immediately and in the long run.
In the short term, people suffer from intense pain due to the sores, made worse by the rotting nature of the affected tissue.
There’s a high risk of infection as the damaged tissue becomes a perfect place for harmful germs to grow.
The danger is increased by the harmful effects of the drug, which not only harms the skin but also weakens the body’s natural defenses.
In the long term, the outlook isn’t good.
Scarring is a common outcome, leaving a lasting mark of the physical and emotional suffering experienced.
Beyond the appearance, the risk of widespread infections is serious.
With the skin’s protective layer damaged, infections can enter the body more easily, possibly leading to serious health problems.
The close network of veins and arteries near where the drug was injected increases the risk of complications, as any disruption to blood flow can cause major issues.
Together, these dangers highlight the need to treat Tranq-induced sores seriously, with immediate medical care and wider efforts to address addiction.
| Aspect | Short-term Effects | Long-term Effects |
|---|---|---|
| Pain | Immediate, acute pain at the injection site, ranging from mild irritation to severe discomfort. | Chronic pain due to scarring, nerve damage, or other complications arising from prolonged use. |
| Risk of Infections | Increased risk of localized bacterial infections at the injection site due to non-sterile injection practices. | Heightened risk of systemic infections that can affect internal organs and potentially lead to life-threatening conditions such as sepsis. |
| Scarring | N/A | Permanent scarring due to repetitive injections, poor wound care, and frequent infections affecting both the appearance and function of the affected area. |
| Other Complications | Potential for localized swelling, redness, and inflammation. | Risk of other severe complications like deep vein thrombosis, gangrene, and potential for limb loss due to tissue necrosis. |
Prevalence and Demographics
Tranq misuse has emerged as a pressing concern in specific regions and demographics.
The Drug Enforcement Administration has detected Xylazine in opioids across 48 out of 50 states, with a notably higher prevalence in Maryland.3
According to the CDC, an alarming 80% of opioids examined at eight needle exchange sites in Maryland contained traces of Xylazine.
While comprehensive global statistics continuously evolve, specific areas, particularly urban pockets in the U.S., have reported spikes in Xylazine-related incidents.
Often found as an adulterant in street drugs, particularly opioids such as Fentanyl, its use has been correlated with an uptick in Tranq sores among drug users.
Demographically, Xylazine misuse seems to gravitate toward communities already grappling with high rates of opioid and injection drug use.
The demographic profile varies, but vulnerable populations, including those with limited health and social services access, appear disproportionately affected.
The geographic and demographic patterns of Xylazine misuse underscore the need for targeted interventions and public health initiatives.
Treatment and Prevention Options
Addressing the Tranq sores issue requires a multi-faceted approach that combines medical treatments and preventive measures.
Medical Approaches to Treating Existing Sores:
Wound Care:
Proper cleaning and dressing of the sores are fundamental.
This might involve using antiseptics, topical antibiotics, and dressings that promote healing and prevent secondary bacterial infections.
Antibiotics:
In cases where a secondary bacterial infection is present or a high risk of developing, oral or intravenous antibiotics may be prescribed.
Pain Management:
Pain associated with these sores can be significant.
Over-the-counter pain relievers or prescribed pain medications can help manage discomfort.
However, careful consideration is needed when prescribing narcotics for individuals with a history of substance misuse.
Debridement:
In severe cases with significant necrosis (dead tissue), a surgical procedure to remove the necrotic tissue might be necessary.
This helps reduce the risk of further complications and promotes healing.
Skin Grafts or Reconstruction:
Surgical intervention in the form of skin grafts might be necessary for extensive or deep sores that don’t heal with conservative treatment.
Strategies to Prevent the Formation of These Sores in Users
Education:
Informing users about the risks associated with Xylazine and the potential for developing these painful sores can be a deterrent.
Harm reduction strategies that educate about safer drug use practices can also play a role.
Clean Injection Practices:
While the best prevention is abstaining, those who continue to use should be advised on clean injection practices to reduce the risk of infections and complications.
Access to Sterile Supplies:
Access to clean needles, syringes, and other supplies can reduce the chances of complications from injections.
Treatment and Rehabilitation:
Encouraging and facilitating access to drug rehabilitation programs can help individuals quit or reduce their drug use, decreasing the risk of Tranq sores.
Emphasis on the Importance of Seeking Medical Attention
Prompt medical intervention can prevent the progression of these sores and reduce the risk of long-term complications.
Individuals should seek medical attention at the earliest signs of skin complications.
Tranq sores can also indicate broader health concerns, including potential systemic effects of Xylazine or other misused substances.
Thus, medical evaluation is crucial for the sores and the individual’s overall health.
Regular check-ups and follow-ups can ensure that the sores are healing correctly and that the individual receives adequate care and support for any underlying substance misuse issues.
In sum, while treatment addresses the immediate concerns associated with Tranq sores, prevention emphasizes the broader issues related to drug misuse and the importance of holistic care.
Addressing the Broader Issue: Tranq Misuse
Combatting the illicit use of Xylazine demands a multi-sectoral approach beyond merely treating its physical manifestations.
Key strategies include tighter regulations on the sale and distribution of Xylazine, ensuring it doesn’t easily divert from its legitimate veterinary use to the streets.
Healthcare professionals play a pivotal role by identifying and assisting patients showing signs of Xylazine misuse, providing necessary treatments, and referring them to rehabilitation services.
They can also raise awareness about the dangers of this substance through community outreach.
On the other hand, law enforcement can intensify efforts to crack down on the illegal distribution of Xylazine, ensuring that those distributing and profiting from its illicit sale are held accountable.
Furthermore, community-based initiatives can offer support networks, educational programs, and resources for those affected, fostering a collective approach to curbing the misuse of Xylazine.
In essence, a united front comprising healthcare, law enforcement, and community efforts is vital to tackle the challenges of Xylazine misuse effectively.
Hope Amidst The Struggle
The misuse of substances like Xylazine sheds light on the broader and ever-evolving challenges of addiction.
It’s essential to remember that addiction is not a choice or moral failing but a complex interplay of biology, environment, and personal experiences.
Every individual has the capacity for change and growth.
Recovery is a journey, often with its hurdles, but one that leads to renewed hope and a brighter future.
The first step can often be the most challenging and transformative.
Cornerstone Healing Center in Scottsdale, AZ, is available to guide and support those on their journey to sobriety.
Our team specializes in addiction treatment and provides personalized, evidence-based care with compassion.
Remember, hope persists in adversity, and help is just a call away!
Are you worried that you or someone you know may be using Tranq?
Check out our article for important information and tips to stay safe!
Is It ‘Tranq’? How To Know If You Or A Loved One Is Using Xylazine